Congestive heart failure is a heart disease where the heart can not pump sufficient blood needed for the body. It often develops gradually, but the early warning signs are frequently ignored. According to Global Cardiovascular Research, CHF affects over 64 million people worldwide, and many of us have no idea we have it yet, and India already has an estimated 1.3 to 4.6 million heart failure patients, and this burden is expected to grow rapidly, says the Indian Journal of Medical Research.
This blog will help you understand about Congestive Heart failure in simple terms, so you can recognize the signs early and take steps to protect yourself and your loved ones.
Understanding CHF: When the Heart Struggles to Pump Blood
Congestive heart failure (CHF) is used to describe a heart condition where the heart muscle becomes stiff or weak and cannot pump enough blood the body needs to function.
As the heart is unable to pump blood efficiently, fluid starts accumulating in the lungs, legs, feet, or abdomen, causing edema (swelling). This results in symptoms like shortness of breath, rapid weight gain, unusual fatigue, and others
This is a chronic and long-term condition. However, the heart does not stop completely; its pumping efficiency and working capacity gradually decrease over time.
What are the Causes for Congestive Heart Failure?
Some common causes of congestive heart failure are:
- Hypertension (High BP): This puts extra strain on the heart, resulting in the weakening of the heart muscle.
- Diabetes: High blood sugar can damage blood vessels, increasing the risk of heart disease and eventually heart failure.
- Congenital Heart Disease: Some people are born with heart disease and are prone to heart failure later in life.
- Arrhythmia (Irregular Heartbeat): Pumping blood effectively is not possible with an irregular heartbeat. Over time, this can weaken the heart.
- Heart Valve Disease: In case of valve dysfunction, the heart also pumps blood inefficiently.
- Kidney Disease: Kidney problems can cause fluid buildup and increase strain on the heart.
- Alcohol Use: It can damage the heart muscle directly.
- Tobacco: They can damage blood vessels, raise blood pressure, and reduce oxygen supply to the heart.
Other Risk Factors for Congestive Heart Failure are-
- Higher BMI (>30)
- Sedentary Lifestyle
- Age above 60
- More Salt and Fat Intake
- Chemotherapy
Signs and Symptoms of Congestive Heart Failure
The most common symptoms someone can experience are-
- Breathing difficulty – During mild activity or especially when lying flat
- Chest pain – Persistent pain or heaviness in the chest
- Palpitations – Irregular heartbeat when the heart is working more
- Swelling in the legs – Fluid buildup due to poor circulation
- Fatigue – Extreme tiredness even with mild activities
Other Symptoms often appear as CHF progresses-
- Weight gain – sudden gain from fluid retention, not fat
- Persistent Dry cough – caused by fluid in the lungs
- Bloating – fluid accumulation in the abdomen
- Loss of appetite – pressure from fluid buildup affects digestion
- Nausea – due to poor blood flow to the digestive system
Stages of Congestive Heart Failure
The stages of congestive heart failure are classified using two widely accepted systems.
- ACC/AHA Staging System
- NYHA Functional Classification
The ACC/AHA system:
Classifies CHF from Stage A to Stage D based on disease progression.
Stage A: At risk
In this stage, the person has the risk factor/s like BP, cholesterol, diabetes etc. The heart is working properly and the disease is not yet developed.
Stage B: Pre-heart failure
The heart muscle changes due to damage or any structural changes. It may become stiff or thickened, or the heart chambers may become enlarged, or there might have been a heart attack previously.
Stage C: Symptomatic Heart Failure
In this stage, the heart can not pump efficiently, fluid builds up and blood supply to organs decreases. Typical symptoms like shortness of breath, cough, leg swelling, and fatigue start to appear.
Stage D: Advanced Heart Failure
This is the final stage of heart failure. Fluid buildup increases and the ejection fraction is reduced significantly. Patients feel difficulty in doing their daily activities, and they may need frequent hospital visits to get relief.
The earlier congestive heart failure is detected, the easier it becomes to manage and treat it effectively.
The NYHA classification:
If you have Stage C or D heart failure, doctors use the NYHA classification to see how severe your symptoms are and to track how well your treatment is working over time.
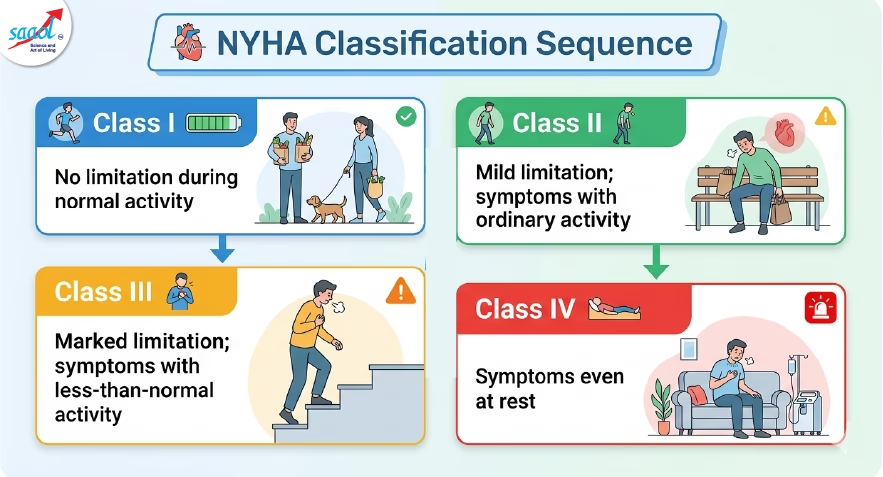
Class I: No limitation during normal activity.
Class II: Mild limitation; symptoms with ordinary activity.
Class III: Marked limitation; symptoms with less-than-normal activity.
Class IV: Symptoms even at rest.
Heart failure can happen at any age. You should not ignore any symptoms that persist. Early detection can help reduce the severity and improve treatment outcomes.
How is CHF Diagnosed?
When you go to the doctor at any stage of heart failure, they use several tests to confirm the diagnosis like-
Echocardiogram: measures the heart’s pumping ability and calculates the ejection fraction (EF).
Electrocardiogram (ECG): checks your heart’s rhythm and electrical activity to spot abnormalities linked to heart failure.
Chest X-ray: helps detect fluid buildup in the lungs, which can be a sign of heart failure
Blood tests: such as BNP helps detect heart failure by showing if your heart is under stress.
Doctors sometimes can also suggest a CT angiogram to check if coronary artery disease is the cause of the heart failure.
What Are the Treatments for Congestive Heart Failure?
If we divide the treatment of heart failure stage-wise. It would be as follows:
Stage A: Managing the Risks
- Medicines to manage risk factors like BP, cholesterol etc
- Healthy lifestyle changes
Stage B: Strengthening the Heart
- Lifestyle management
- Beta-blockers if EF is below 40%
- ACE inhibitors
- EECP on conditions like blocked arteries or chest pain
Stage C: Controlling Symptoms
- Beta-blockers and aldosterone antagonists
- Diuretics to reduce fluid buildup and swelling
- Implantable devices like pacemakers or defibrillators (ICDs) if needed
- EECP Therapy
- Lifestyle and diet changes, weight management
Stage D: Advanced Intervention
- Heart transplantation
- Mechanical circulatory support (LVADs)
- Continuous IV medicines to help the heart pump better
- Palliative care to reduce symptoms and improve comfort and quality of life
EECP Therapy: A Safe, Non-surgical Treatment for Heart Failure
EECP stands for Enhanced External Counterpulsation, an FDA-approved non-invasive therapy that improves blood flow to the heart without surgery, needles, or hospitalization.
When the heart is weak, it struggles to pump enough blood through the body. EECP helps by making that easier.
How Does EECP Support Heart Failure?
EECP does two powerful things for CHF patients:
- It reduces the heart’s workload, so the weak heart doesn’t have to take strain.
- It builds natural bypasses, encouraging the body to grow new blood vessels around blocked ones, improving circulation without surgery.
Over time, the heart grows stronger and symptoms ease.
Can Lifestyle Changes Prevent Heart Failure?
The short answer is yes.
Regular activities like walking, yoga, or light exercise can help lower the risk of heart failure by controlling major risk factors like high blood pressure, diabetes, obesity, and high cholesterol.
Eating low-oil, low-fat foods helps manage weight and cholesterol.
Stress management keeps blood pressure and heart rate stable.
Treatment works best when therapy and lifestyle go hand in hand.
SAAOL Heartcare Delhi, having 30+ years of expertise in non-invasive heart treatment, does it all.
EECP therapy helps the heart pump better, reducing breathlessness, fatigue, and chest pain. On top of that, SAAOL’s expert team helps you with zero-oil cooking, managing stress, and staying active, so your heart keeps getting stronger every day.
If you or a loved one is living with CHF, SAAOL’s EECP program may offer the relief you’ve been looking for.
Key Takeaways
Congestive Heart Failure is concerning, but it is manageable. The earlier you catch it, the better your chances of living a full, active life.
Dr. Vishal Sharma from SAAOL Heartcare Delhi says, “Heart failure can happen at any age. Awareness is the key. Do not ignore regular checkups, especially if you have BP, sugar, or a history of heart disease.”
Do not ignore the signs your body is giving you. With the right treatment plan, including EECP therapy and lifestyle support, recovery is possible.
FAQs
Q1.Can congestive heart failure be reversed?
Yes, you can prevent heart failure only at the early stage with medicines, therapies, and healthy habits. It can not be reversed completely once the symptoms start appearing. But it can be managed by improving heart function with the right treatment and lifestyle changes.
Q2. Should Heart Failure Patients Avoid Exercise?
Not if you do it correctly. You should know which one is appropriate according to your health condition. However, intense exercise without medical guidance can be harmful. Always consult your doctor before starting any exercise routine.
Q3. What does CHF stand for in medical terms?
CHF stands for Congestive Heart Failure, a condition where the heart cannot pump blood efficiently due to fluid building up in the lungs or body, and the patient feels fatigue, chest pain, or breathlessness.
Q4: Is there any difference between heart failure and congestive heart failure?
Yes, there is a minor difference in heart failure and congestive heart failure. Heart failure is a broader term for when the heart cannot pump blood properly. Congestive heart failure (CHF) is a type of heart failure in which fluid builds up in the lungs, legs, or abdomen, causing swelling and shortness of breath.
Q5. How do I know which stage of CHF I’m in?
It depends on the severity of symptoms and the underlying conditions. Must visit a cardiologist to determine your CHF stage. Physical examination, ECG, and echocardiogram are the 1st step to determine. If you are experiencing breathlessness, swelling, or fatigue, get evaluated as soon as possible.


